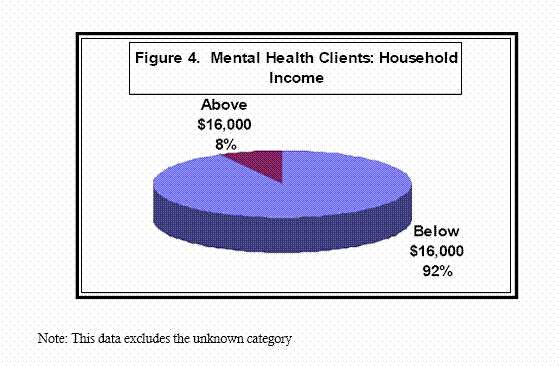In the last few decades, the number of Americans classified as having mental disorders saw a dramatic increase, as did the number of people seeking and receiving mental health services. This increase can be attributed to the growing understanding that mental illness is a treatable disease, as well as the lessening of the stigma surrounding mental illness. Improved diagnoses, innovative therapies, and radically new medications, coupled with recent breakthrough prescription medications with higher effectiveness and fewer side effects have also contributed to this trend, which is now evident in Nevada and throughout the nation. Despite these advances, delivering mental health services to the affected population remains a major challenge requiring the concerted efforts of government, local communities, and families of consumers of mental health services.
Federal involvement in mental health policy has grown in the last decade, pushing the public mental health systems in a new direction. Perhaps the most important development in this respect has been the creation of the Substance Abuse and Mental Health Services Administration (SAMHSA), http://www.samhsa.gov/, established by Congress in 1992. Other landmark developments in the field of mental health include a 1999 U.S. Surgeon General report, http://www.surgeongeneral.gov/library/reports.htm, highlighting mental health as a major national public health issue; a United States Supreme Court landmark decision appearing in the same year, commonly referred to as Olmstead, that established a constitutional mandate to provide mental health treatment to individuals in the least restrictive environment appropriate to their condition; and the creation in 2002 of the federal New Freedom Commission on Mental Health, http://www.mentalhealthcommission.gov/, that promoted community-based models of mental health care. Mirroring these national developments is the Nevada Mental Health Plan Implementation Commission Report, http://www.leg.state.nv.us/lcb/research/05InterimReports/Bulletin05-08.pdf, which laid groundwork for the provision of mental health services in the state. The overall shift away from inpatient treatment is a national trend that has also been evident in Nevada (State Profile Highlights, 2005).
While federal policy has had a major influence on the delivery of mental health services, the responsibility for the organization and dispensation of public mental health in Nevada has, by statute, been vested in the state government. The present report reviews the quality of mental health care in the Silver State. After a brief historical overview, we identify the most urgent needs, point to work ahead, and describe community resources available in our state to individuals and families with mental health problems.
Historical Overview
Nevada’s mental health system traces its roots to 1868 when the Nevada territory became a state (Chanslor, 1968). Four years after achieving statehood, the Nevada Legislature authorized a contract with the State of California for the admission and care of insane residents in Nevada. In 1871, the Nevada legislature created the first “Board of Commissioners ” to keep control of and provide care for the insane. Comprised of the Governor and a treasurer, this first board authorized the building of Nevada’s first state asylum, which was completed in 1882. Most of these original structures remain standing, and many are still in use. In 1883, 148 “inmates” were transferred from Stockton California to Nevada’s new hospital. By the 1880’s, the need for a state hospital became apparent, as some early settlers experienced fatigue and mental illnesses while traversing the United States during the western expansion. Nevada records show that even the bravest and most courageous families were not immune to mental illness.
In one of the very few historic reviews of mental health services in Nevada, Pillard ( 1979) identified three characteristics of Nevada’s system: (1) marked fluctuations in service capacity; (2) a lack of public supervision or independent professional review of mental health programs; and (3) absence of long-term planning. The Nevada system of mental care first appeared in Northern Nevada, starting with a single hospital in Reno that was called at the time the Nevada Insane Asylum. In 1895, the name changed to the Nevada Hospital for Mental Diseases. In the early 1900’s, patients stayed almost entirely within the confines of this institution. Many worked on the hospital ground, with the family members helping along. In time, this “asylum” evolved into what is now the Northern Nevada Adult Mental Health Services.
Notable improvements occurred throughout the 1940’ s thanks to the legal actions that produced better treatment activities, separate programs for men and women, appointments of guardians, and the allowance of “voluntary” commitments. Beginning in 1943, the Superintendent was no longer required to be a physician. In 1944, conditions in the hospital reached a level that required a legislative investigation, which brought in its wake structural changes in the system. In the mid 1940’s, a new board of Commissioners for the Indigent Insane was created to assist the governor. T he commission elected a state Superintendent for the Hospital. It is interesting to note that, until the late 1930’s, many patients lived most of their lives in the hospital and were actually buried on the campus. This practice was discontinued in the 1940’s.
The mental health care system in Southern Nevada is of much more recent vintage. The Community Mental Health Act passed under the administration of President John F. K ennedy paved the way for Southern Nevada to develop its first mental health outpatient clinics in the mid 1960’s, nearly 100 years after Northern Nevada blazed the trail. Around 1975, the first public psychiatric hospital opened its doors in Southern Nevada (C. Brandenburg, Personal Communication, January 2006).
As the above overview suggests, the mental health delivery systems differed substantially in southern and northern parts of the Silver State. Whereas in northern Nevada, mental health services evolved from a hospital based institutional setting, in southern Nevada the mental health service system relied primarily on community-based programs. And when the federal government announced its policy favoring community-based services in the 1960’s, this shift caused more cultural problems and organizational changes in the state’s northern regions.
Reflecting a new attitude toward mental illness as a component of public health and human development, the division’s name was changed in 1998 from the obsolete “Mental Hygiene and Mental Retardation” to the current “Mental Health and Developmental Services.” Modern day governance of Nevada’s public mental health system is vested in the Division Administrator appointed by Governor. Dr. Carlos Brandenburg currently serves as the Mental Health & Developmental Services Administrator in Nevada.
Problems and Delays in Service Delivery
In a 1995 article published in the Nevada Public Affairs Review, Brian Lahren, former Administrator of the state Division of Mental Hygiene and Mental Retardation (now the Division of Mental Health and Developmental Services), traced the deterioration in Nevada mental health services over more than a decade. This decline started in 1983 when the state, facing financial exigency, cut funding for mental health services. After a temporary reversal in the late 1980’s, the state mental health budget plummeted again in 1991-92 when the budget was cut by a crippling 12%. Adjusted for inflation and population growth, this reduction led to an effective 40% drop in the overall funds available to treat mentally ill residents of the state. While T the situation improved in the late 1990’s, but state mental health services have never fully recovered from the precipitous decline of the prior decade.
Several historical factors have contributed to the critical state of affairs in the Nevada mental health delivery system, including a rather unique statewide delivery structure in which the state has been the sole provider and a primary source of funding for public agencies delivering mental health services. Historically, Nevada lacked acute care facilities that were designed as part of the public mental health system, with Southern Nevada completely lacking a psychiatric acute care infrastructure. The Silver Sate was also uniquely vulnerable to budget cuts due to the personnel-intensive nature of mental health services and the relatively powerless political voices of those most affected by the cuts. We also should note the unprecedented population growth, particularly in Southern Nevada. For 18 consecutive years, Nevada has been the fastest growing state in the nation. This population explosion has led to a dramatic increase in consumers needing mental health services. Adding to the mental health delivery crisis in the state was the decision by private providers, particularly psychiatric inpatient facilities, to reduce or eliminate their beds at the time when state agencies were already losing ground in their ability to meet demand for services.
A recent report by the National Alliance of the Mentally Ill (2006) ranked all 50 public mental health systems. In Nevada, the grade received was a disappointing “D-“. This NAMI report went on to indicate that
- Nevada ranks very poorly – 37th – in overall mental health spending, and 36th in per capita MH expenditures, while at the same time ranking 4th in the nation for suicide rates.
In spite of acknowledged long-standing system shortcomings in Nevada’s system, the NAMI report went on to discuss outstanding strengths and challenges in Nevada’s public system of mental health in 2006, which included;
Innovations
- State funded mental health courts
- Transparency, demonstrated by self-reported data posted on the MHDS website
- Efforts to reduce restraints and seclusions in hospitals
- Funding increases for emergency room and jail diversion programs
Urgent needs
- Overflowing emergency rooms, particularly in Las Vegas
- Implementation of evidence based practices an Act programs
- Supportive housing options especially in rural areas
NAMI is not the only source to note the persistent reports of long waits to obtain services in Southern Nevada. In fact, delays in access to Southern Nevada’s only public psychiatric facility have continued particularly since Clark County Manager Thom Reilly’s declaration of a state of emergency in July of 2004. Because of the statutory requirement that consumers must receive a medical clearance prior to acceptance by a state psychiatric facility, local hospitals were overwhelmed by the influx of psychiatric patients waiting for access to Southern Nevada Adult Mental Health Services (SNAMHS). Hundreds of psychiatric patients were warehoused in local emergency rooms, claiming nearly one-third of the total number of emergency beds.
While the news might have been startling to the public, the problem had become chronic and all too familiar to those working in the Nevada public mental health system. In fact, it had been growing for more than a decade.
The long waits in Southern Nevada have impacted not just those with an acute mental health crisis. Emergency room operations are designed to turn patients over approximately every 4 hours, either by releasing them to the streets or admitting to another hospital department. Mental health patients may occupy the same bed for 27 times that length, which means that each patient potentially displaces approximately 26 emergency patients. Multiply the number of displaced by 70 – the number of patients held for sustained periods – and the crisis for acute medical care becomes apparent. In December 2005, Nevada had almost 1,600 people waiting at some time in the Clark County emergency rooms to be admitted to the mental health system (see Appendix for detail).
Reports found in the publications section of the MHDS, http://mhds.state.nv.us/sn/index.shtml, reveal a crying gap between the psychiatric needs and available services. The emergency rooms in Las Vegas Valley are overwhelmed by the number of psychiatric patients who are held for extended times in emergency room facilities because there are insufficient Psychiatric Emergency Beds and Psychiatric Acute Care Beds at SNAMHS.
- In 2003, the patient to psychiatrist ratio in Nevada was approximately 700:1, as opposed to the target of 345:1. In the same year, there were 36 private psychiatric beds for the entire Clark County region with a population of 1,620,748.
- The State of Nevada estimated that in December 2005, 1595 people waited on average of 85 hours in hospital emergency rooms for access to the public mental hospital (Crowe, 2006).
- As many as 50% of those held in hospital emergency departments are eventually released to the streets without receiving any treatment.
- State officials estimate that about 40% of all clients leave the state psychiatric emergency clinic without being served because of intolerably long waits.
Southern Nevada has been losing ground for years in mental health delivery services. In the past five years alone, Clark County lost 133 private beds. The number of psychiatric beds in private facilities has been dropping nation-wide due to emphasis on the more lucrative general medical surgical facilities. The decline was especially precipitous in Nevada as a whole , where it produc ed ing more adverse consequences.
With strong leadership from Governor Guinn and the Nevada State Legislature, MHDS managed to secured major budget and staff increases in 2003, which significantly improved the Division’s ability to provide mental health services in the state.
- The most recent 2005 legislative session marked the largest budget increase to date at over 47%. In the MHDS State Fiscal Year (SFY) 2005, the Legislature-approved budget of $194,976,376, of which $99,876,254 was dedicated to mental health services, $91,647,821 was budgeted for developmental services, and the remaining $3,452,301 was earmarked for administration (see Appendix for budgetary and staffing details).
- Additional mental health allocations of over $19.5 million made through Assembly Bill (AB) 175, sponsored by Assemblywoman Sheila Leslie, resulted in total budget growth for MHDS of 51.6% during SFY 2006 – 2007 (see below).
By the start of the 2005 legislative session, the Guinn Administration had already taken crucial steps to address the growing crisis. Foremost was the decision to move the building of a new psychiatric facility in Southern Nevada to the top of the state’s list of capital improvements. With bi-partisan leadership provided in particular principally urged by Governor Guinn and Assemblywoman Sheila Leslie, the Nevada Legislature responded with the unprecedented 51.60% ($91 million) increase in mental health funding. Additio nally, AB 175 further added 12.6 million for expanded mental health crisis services, and mental health courts.
Although the three principal state facilities
– SNAMHS, NNAMHS, and Rural Clinics Community Mental Health Centers (RC) – all received substantial increases, the lion’s share of the increase was used to mitigate the Southern Nevada emergency room crisis. Funding also aided the expansion of the Clark County Mental Health Court, the continuation of a community triage center, and the establishment of a temporary 50 bed 50-bed overflow treatment facility (Westcare). These budget increases and organizational measures bode well for the mental health services delivery in the three primary regions of the state. Yet even these boosts failed to stem the crisis in southern Nevada.
Demand for Mental Health Services
To appreciate the magnitude of the problem, consider the following data pertaining to the mental health needs in our state:
- In a 2003 report of the Kaiser Family Foundation, http://www.kff.org/, Nevada ranked 1st (worst) in the nation with 42% of the population reporting poor mental health in the prior 30 days.
- At the other end of the spectrum, states reporting low incidence of mental illness included Hawaii (19.3%) and North Carolina (24.8%). Neighboring California ranked relatively poorly in third place behind Nevada with 40.9% reporting poor mental health.
- In 2004, the national average of publicly funded psychiatric inpatient beds was 33 per 100,000 residents. By comparison, Nevada had some 4.5 beds per 100,000. (Even with the significant anticipated increases, the ratio in Clark County would grow just to 21:100,000).
- The 2004 Center for Mental Health Services report ranked Nevada as the worst among 15 western states for mental illness prevalence. The study projected that 23.7% of Nevada residents will have a diagnosable mental disorder at some point in their lifetimes.
Estimates of the prevalence of individuals in the population who have serious disorders in a given year are useful in planning and generating performance indicators. A direct survey of the population is the best way to make these estimates, but a well-designed survey is expensive. Special techniques have been developed that allow indirect inferences from national epidemiological studies regarding the trends at the county. The federal government has funded two major national epidemiological surveys for adults: the Epidemiological Catchment Area Survey and the National Comorbidity Survey. These surveys used structured diagnostic interviews to obtain detailed information about prevalence rates for mental disorder in various sociodemographic groups (age, sex, race, ethnicity, education, poverty level, marital status, etc.)
There have been a number of studies of the mental health of children and adolescents, although these fall far short of the massive scope of surveys such as the ECA and the NCS. Estimation relies heavily on the methods of the CMHS reports, Estimation Methodology for Children With a Serious Emotional Disturbance (SED) (1997), and Children With Serious Emotional Disturbance; Estimation Methodology (1998).
Results from these studies are applied to census data to generate estimates. At the national level, epidemiologists have applied this technology for several states including Colorado, Nebraska, South Dakota, Washington, Washington D.C., and Wyoming. For Nevada, this source data was updated using the 2003 Nevada Census data (July 1, 2003, Estimates). This results in Nevada having the most up-to-date and accurate prevalence estimated available nationally. Estimates were made for children and adolescents with serious emotional disturbance (SED) and adults with serious mental illness (SMI). Estimates generated were based on the National Comorbidity Survey for adults, the Epidemiological Catchment Area survey for the elderly. Both studies were used in combination with other research and expert opinion for estimates for children and adolescents (Kessler et al, 1996).
The most serious mental illnesses are generally classified into two service strata, referred to as those with serious mental illness (SMI) or serious and persistent mental illnesses (SP MI). Unlike oth er states in the region, Nevada focuses on provision o f services to those who qualify for the SPMI category. SPMI populations are the most difficult and expensive to servi ce, as this generally include s all aspects of life, money management, residential supports, and use of the most expensive medications. Other states often provide less urgent services to a wider strat a of the general population, sometimes providing services to milder and situat ional disorders, for example.
Although this prevalence data is subject to varying interpretations, it we may be conclude d that it they reflects a public system focused largely mostly on serving just those consumers with the most serious and persistent mental illness. In addition, the picture suggests a significant focus on crisis response rather than on health maintenance and prevention. Further, the lack of adequate numbers of community-based programs and the location of state hospitals at just two locations in the state, one in Clark County and the other in Washoe, may result in higher rates of hospitalization and treatment at greater distance from one’s home
Estimation tables were developed for counties and aggregated to service areas and the State (Holzer, 2004). Tables were broken down by age, gender, race/ethnicity, poverty level, and residence type.
- Nevada has fewer public psychiatric beds per 100,000 population than Oregon, Utah, Idaho, or California. Nevada ranks 43 nationally and is significantly lower than any of these states.
- Nevada has fewer public psychiatric beds per capita than the surrounding states. To meet the national avg. ratio of 33 psychiatric beds per 100,000, the new hospital would need to provide 511 beds (Overview of Plans for the New Psychiatric Hospital In Las Vegas, 2004).
- The total number of available psychiatric beds in the private community has dropped dramatically since 2000. There are insufficient private acute psychiatric beds in Las Vegas Valley to provide services to the people living there. This has caused a 44% drop in available private adult psychiatric beds in less than 3 years.
- Nevada spends much less than the national average on Mental Health including funding for hospital services (Facts about the New State Psychiatric Hospital in Las Vegas Valley, 2004).
Mental Health Care Delivery in Nevada
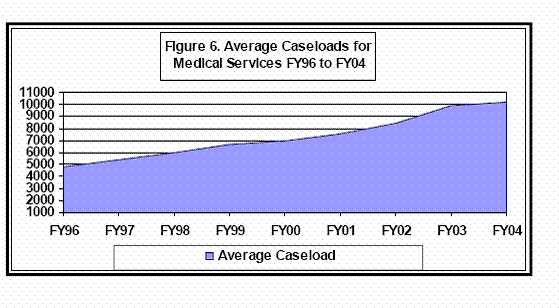
The Division of Mental Health and Developmental Services (MHDS) will provide services to approximately 25,000 Nevadans in State fiscal year (SFY) 2005 (Facts About The New State Psychiatric Hospital in Las Vegas Valley, 2004). In addition to serving these direct consumers, MHDS works with many stakeholders including family members, advocates, service providers, legislators, law enforcement, and the public . As a result of these diverse interests, the issues facing MHDS are complex and require input from many different perspectives. The underlying thread of unity in this diverse system, however, is the commitment of all stakeholders to a public mental health and developmental services system that meets the needs of Nevada’s citizens.
MHDS is responsible for the operation of State-funded outpatient community mental health programs, psychiatric inpatient programs, mental health forensic services, and all developmental services programs and facilities. By statute, the Division is responsible for planning, administration, policy setting, monitoring, and budget development of all State-funded mental health and developmental services programs. MHDS Administration is also directly involved in decisions regarding agency structure, staffing, program, and budget development.
The mission of the Division is to develop and operate programs that assist individuals who have mental illness or developmental disabilities to live as independently as possible. The Division is obliged to offer care regardless of ability to pay, provide services in the least restrictive environment, base services upon individual needs, and honor clients’ rights. MHDS is committed to providing cost-effective services that ensure consumer and citizen safety, can be readily accessed by all persons in need, are consumer-driven, and promote self-sufficiency.
Appointed by the Governor, the Division Administrator relies on the oversight and direction of stakeholders as represented in several advisory groups:
Commission on Mental Health and Developmental Services (MHDS Commission). The MHDS Commission is appointed by the Governor to articulate policies and ensure effective administration of services for persons with mental illness, mental retardation, and related conditions. The Commission has several powers related to the oversight of programs within the Division.
Local Advisory Boards. The MHDS Commission has created advisory boards in Washoe and Clark Counties and makes appointments to these boards from stakeholders in the community. The boards serve to provide information to the Commission regarding service needs, public input, and other issues pertaining to mental health.
Mental Health Planning Advisory Council (MHPAC). Public Law 102-321 mandates that stakeholders, including mental health consumers, their family members, and parents of children with SED must be involved in mental health planning efforts related to the block grant through membership in planning advisory councils (PACs). To this end, the State of Nevada Mental Health Planning Advisory Council (MHPAC) was established in 1989. PACs have three federally mandated duties: (1) To review the Mental Health Block Grant Plan and make recommendations; (2) to serve as an advocate for adults with a serious mental illness, children with a serious emotional disturbance, and other individuals with mental illnesses; and (3) t o monitor, review, and evaluate at least once each year the allocation and adequacy of mental health services within the state.
Administration and services are organized into three regions: north, south, and rural. Four agencies deliver mental health care in the state:
Northern Nevada Adult Mental Health Services (NNAMHS) – north. This inpatient psychiatric hospital provides a variety of outpatient, community-based services.
Lake’s Crossing Center – north. Co-located with NNAMHS, this is the State’s facility for criminal offenders with mental illness.
Southern Nevada Adult Mental Health Services (SNAMHS) – south. This is a n inpatient psychiatric hospital offering a variety of outpatient, community-based services through four community mental health centers.
Rural Clinics – rural. This organization operates a network of 18 community mental health centers in the state’s rural counties. In addition to providing services to adults with SMI, Rural Clinics provides services to children with SED in the rural areas in cooperation with DCFS.
Although much media attention has been focused on the hospital bed shortage in Southern Nevada, it would be unfair to conclude that the mental health services system is functioning adequately throughout the rest of the state. In large measure, the psychiatric bed shortage crisis reflects the lack of adequate community-based outpatient and prevention resources. Since responsibility for public mental health services rests exclusively by statute with the state, counties are dependent upon state resources to provide such services. According to State of Nevada sources, in FY04
- 80% of Nevada’s mental health spending (approximately $69 million) came from the state general fund, 11% was attributable to federal sources, and 9% was paid by other sources (with less than 1% paid by clients).
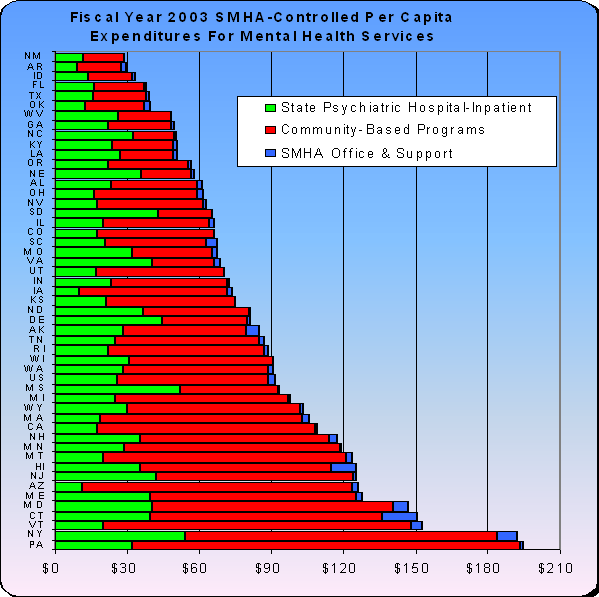
State-by-state comparisons are difficult to make because state delivery systems differ in significant ways, yet some noteworthy trends can be discerned from a MHDS July 2005 report by Donald R. Karr and Laura Valentine summarizing FY03 and FY04 multi state data (Karr and Valentine, 2005) reached the following conclusion:
- Although Nevada fares quite well in mental health spending on a per-consumer basis ($5 ,067 compared to $4 ,917 nationally), when mental health expenditures are spread across the entire state population, Nevada ranks below most of its neighbors and well below the national average ($59 per 1,000 in population versus $92 nationally).
- Nevada state agencies serve a smaller portion of resident consumers than the national average (11.7 consumers per 1,000 versus 18.6 nationally).
- The percentage of mental health consumers served in psychiatric hospitals significantly exceeds the national average. In fact, the proportion of Nevada consumers served in state psychiatric hospitals is more than twice as high as its neighbors and the U.S. as a whole (7.7% compared to 3% nationally).
- With respect to the provision of funding for community-based services, Nevada ranks below all of its neighboring states (Utah, Arizona , and California), one exception being Oregon, if we consider per client spending (see Appendix for detail) National comparative statistics are not available).
- As to percentages of consumers being served in their own neighborhoods, Nevada again reflects substantial disparity with most of its neighbors and with the United States as a whole (88% compared to 96%).
Children and Youth with Mental Disorders
The consequences of unaddressed severe emotional disturbance (SED) in children and youth include school failure and entanglement with the criminal justice system. Understanding the dimensions of mental health needs for th is e young segment of our population is crucially important. Although we do not have reliable statewide data for the general school age population, we have some information from which we can reasonably extrapolate. In 2004, the Clark County Children’s Mental Health Consortium, http://www.dcfs.state.nv.us/Plans/CCCMH_Annual_Plan_2004.pdf, sampled elementary students in the Clark County School District. The major findings are summarized below:
- Approximately 20% of the children required some level of mental health care, a number mirroring national data. Although studies have not yet been conducted for Washoe County and the rural areas, there is no reason to doubt the 20% figure as a good benchmark.
- About 13% of the students sampled required targeted intervention, while the 6% were in need of intensive services, and; the remainder would benefit from school support programs.
- Other Nevada studies which focus on relating to youth in state and local juvenile justice residential programs have found that the percentage with a specific mental health diagnosis can reach 40 or 50%.
The level of unmet needs in the general population, as well as the child welfare and juvenile justice systems, is striking:
- Some 83% of the children sampled in the Clark County School District were not getting the level of services needed. A full 63% of those in need were getting no services at all.
- In the child welfare system, 70% were getting less than adequate level of service, and 44% of youngsters with psychiatric needs received no treatment. Similar numbers were reported by the Nevada juvenile justice system.
Key to addressing mental health problems in children and youth are early identification and quick referral to obtaining appropriate services. Assuring access to such resources can be particularly challenging in the rural communities. Nevertheless, the introduction of wrap-around services (WIN) throughout the state – the provision of a range of comprehensive community-based supports for the child and family – has shown promise for helping young people achieve good mental health without having to leave their communities.
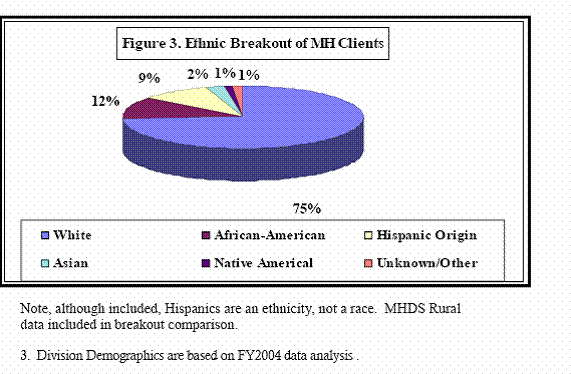
Socio-Demographic Factors in Mental Health
Individuals suffering from serious mental illness are further burdened with a range of other hardships and obstacles to quality of life.
- The MHDS The State of Nevada 2004 Biennial Report, http://mhds.state.nv.us/pdfs/BiennialReport2004.pdf, indicates that approximately one third of state clients have never been married, and a majority identify themselves as single.
- A 2005 MHDS report (Karr and Valentine, 2005) revealed According to the 2005 that , just 18% of Nevada mental health consumers are in competitive employment, compared to about 22% nationally.
- It is estimated that 92% of all clients earn below $16,000 annually, compared to about 10% of the general population in Nevada living below the poverty level.
- The 2003 data from Clark County Detention Center points out that approximately 20% of the inmate population have a serious mental illness (SMI). This number understates the extent of the problem, since it does not include inmates awaiting screening and those on suicide watch.
- The last estimate is somewhat higher than the national figure of 16.9% used by the United States Department of Justice. It is also known that a substantial percentage of inmates in the Nevada State Department of Corrections have SMI.
- Suicidal behavior is known to correlate with certain psychiatric disorders; over the last couple of decades, Nevada ranked at the top of the nation for per capita suicides, dropping to fourth place in 2003.
- Nevada also ranks higher than average in incidence of tobacco, alcohol, and marijuana use, behaviors that are known to bear relevance to correlate with mental illness rates.
- Occupational stressors, social isolation, single status, poverty, homelessness, migration, rapid social change, and other social factors correlate strongly with increase in mental illness rates.
As many of these factors seem to be prevalent in Southern Nevada, more systematic research research that is more systematic is needed to assess their separate and cumulative effects. We need more precise and systematic data on the distribution of patients by mental illness categories, age, ethnicity, social class, gender, race, occupation, and other important social-demographic variables which are known to correlate with mental illness.
Prospects for the Future and Recommendations
The MHDS 2004 Needs Assessment provides a progress report on unmet needs identified in the previous 2002 report for central office improvement. The 2002 report singled out seven areas of unmet needs. Substantial progress was made within the following six areas (Valentine, 2004):
- Agency accreditation
- State participation in the Western Interstate Commission for Higher Education (WICHE)
- Management information system conversion and upgrade
- Disaster preparedness
- Statewide Consumer Assistance Program (CAP)
- Workforce recruitment and retention especially in rural Nevada
The future efforts requiring long-term investment(s) include several key areas.
Adequate Hospital Capacity
The anticipated opening of a 190-bed state psychiatric hospital in Southern Nevada with full staffing is an essential first step to alleviating the immediate crisis in service delivery. Regrettably, an attempt to obtain funding for a projected $18 million on-site medical screening capability at the state facility failed. Such an investment, which would largely be a one-time expense, would have increased the likelihood for expedited assessment and treatment of those in need of psychiatric services.
- In 1996, the National Center for Mental Health Services (CMHS) determined that the national average of state hospital psychiatric beds per 100,000 population was 33.
- In comparison, Clark County is seriously under-bedded with only 4.5 psychiatric beds per 100,000.
- To meet the national avg. ratio of 33 psychiatric beds per 100,000, the new hospital would need to provide 511 beds.
Continued Commitment to Best Medication
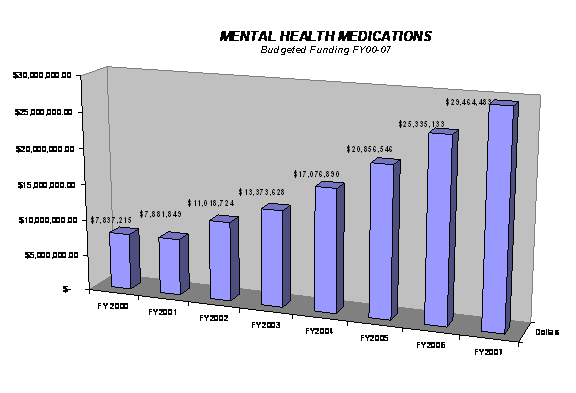
M edications used to treat emotional disorders are often referred to as psychotropic medications. In the 1990s, new psychotropic medications began to enter commercial markets . These new generat ion medication s are generally easier to admini ster and have fewer side effects. Use of these modern medicines consistent with evidence-based practices have proven to be substa nt ially more effective than treatments available prior to 1990. Continued commitment to best medication. The state’s continued commitment to provide a new generati on of psychotropic medications in recent years has benefited many patients. In addition, And the implementation of mental health courts in the two urban areas has shown promise in addressing problems with treatment compliance that could otherwise lead to involvement in the criminal justice system. The provision of state funds to permit expansion of the mental health court in Southern Nevada will make a significant impact on the additional 75 clients served and will also decrease jail and hospital emergency bed usage. (See Appendix for a chart summarizing the funding levels for MHDS medication budget).
Round-the-Clock Crisis Centers
Crisis centers are small programs involving personnel trained to deal with people in acute distress. Such centers specialize in round-the-c lock services for patients brought in by my family members, law enforcement, or themselves so they can be observed and sorted out and transported to the most appropriate treatment facility (a process referred to as “triage”). In spite of these promising developments, a minimally acceptable mental health system is yet to be achieved. There is a compelling need for adequate crisis units operating on a 24/7 basis, and where clients can walk in or be dropped off by family, friends or law enforcement officers to get prompt assessment and treatment. Long term secure funding for such facilities is essential.
Use of Evidence Based Practices ccc (EBP’s)
EBP’s include interventions and techniques whose effectiveness is substantiated by valid and reliable data. Consistent use of these clinical practices statewide will require additional staff training and data reporting. Currently, MHDS does not have adequate infrastructure or training capacity to undertake most of these EBPS. Nonetheless, to the extend that resources allow, Nevada uses the following EBP techniques:
- Assertive Community Treatment
- Supported Employment
- Supported Housing
- Family Psycho-education
- Integrated Treatment for Co-occurring Disorders
- Illness Management
- Medication Management
Accessible Community- Based Services
Community based services cover all the services not provided in hospitals but available in neighborhoods and the community at large. Such community services can include outpatient clinics, medication clinics, medical and dental care, social services, child and respite care, etc. Other programs, such as drop in centers and clubhouses, are also community programs where people can visit informally, without any appointments, and where they can safely interact with peers, neighbors, and mentors. Such services are crucial to compliment adequate inpatient programs so that people do not return to hospitals unnecessarily. More importantly, there is a need to continue to expand services so that the system can adequately shift from crisis-oriented , hospital-based investment of funds to the longer term community-based service approach that will assure mental health consumers adequate access to counseling and prescription services before a crisis arises. Securing f unding for medication clinics with adequate staffing to encourage medication compliance is an important step that will improve quality of mental health services in Nevada.
Community-based services must have flexible hours to allow adequate access. It is important, also, to take into account transportation needs of clients unable to drive or traveling long distances, especially in rural areas. Residential programs are a crucial part of the system of community - based services. In spite of additional funding in recent years, adequate residential supports are still lacking for people with SPMI.
Lowering Language and Other Cultural Barriers
As the Surgeon General suggests, culture matters tremendously in every aspect of mental illness. Since Latinos represent a growing segment of the Southern Nevada population, much more needs to be accomplished to ensure that they and members of other minority groups have access to programs, agencies, and personnel which are sensitive to cultural differences with regard to mental illness. Written information should be available in their languages, and the provision of mental health services to these communities will require both bilingual mental health professionals and the recruitment and training of members of these communities.
Attention to Senior Citizens’ Needs
Since senior citizens have different mental health needs than younger ones, more precise information about rates and types of mental illness by age categories must be gathered to efficiently administer mental health services for this special population. Given the state of Nevada growing attractiveness to retirees, this concern will increase in importance with the passage of time.
In partnership with the Division of Aging, MHDS provides outreach for seniors with SMI in the southern region through SNAMHS and in the northern region through SNAMHS. The Senior Mental Health Outreach Program provides services to adults ages 60 and older who are experiencing symptoms of mental illness, with the primary goal to identify, evaluate, and provide effective mental health care through community outreach.
Direct care services, including evaluation, counseling, and s ervice c oordination (case management), are primarily offered to seniors in their own home. Clinicians are able to complete intakes for new clients in the field. This program helps secure access to mental health care by seniors lacking in transportation or encountering physical and medical obstacles to receiving services at traditional mental health facilities. Often community professionals, neighbors, family members, and others involved with seniors will suspect a need for mental health care and will refer the person to the program, as seniors are sometimes reluctant to go to an office to see a mental health service provider.
Integrated Treatment for Co-occurring Disorders
Co-o ccurring diso rders refer to the diagnosis of substance abuse for people who already have a mental illness. Substance abuse is pred o minat e in mentally ill population s and sometimes is referred to as “self-medication.” Although Nevada has begun to recognize the importance of treating co-occurring disorders (e.g., mental illness and substance abuse) in a seamless manner, there is much to be done to make adequate programs available across the state.
Beyond meeting fundamental treatment needs, we have to maintain a sustained attention much remains to be done to promote productivity and other quality of life factors that Nevada consumers deserve. Adequate housing and day centers for use by the seriously mentally ill are scarce. AndDespite the critical needs that are yet to be met, met, it is not too early to begin start asking when job training job-training services will be made fully available to the economically most vulnerable segments of our population. Until these basic resources are secured, a substantial portion of Nevada ’s consumers of mental health services will be held back prevented from achieving their potential as productive citizens.
Interest in integrated mental health programs with substance abuse system is furth er evidenced in the passage in 2004 of Assembly Bill 2 that transferred the Bureau of Alcohol and Drug Abuse (BADA) into MHDS effective July 2007. Planning is underway to merge these previously separate agencies to further realize integrated services for co-occurring disorders.
Mental Health Courts
In November 2001, under the leadership of Assemblywoman Sheila Leslie, Judge Peter Breen, and advocate Rosetta Johnson, a mental health court was established in Washoe County, through which offenders with mental illness volunteering to appear before the Court take part in a mental health treatment program instead of receiving jail time for criminal offenses. Offenders diverted to the Court have long histories of criminal offenses and hospitalization with concomitant resistance to mental health treatment. The Court is serving to assist these individuals to get the treatment they need, thereby keeping them out of jails and hospitals. Participants in the program must check in with the Court regularly. Recent data shows the Court has significantly reduced repeat arrests and hospitalizations. In December 2003, a mental health court was established in the southern region of the state to make this program available to Nevada ’s largest population center.
Disaster Response and Bioterrorism Preparedness Programs
The Division of Mental Health and Developmental Services (MHDS) currently has a statewide mental health disaster response plan in place. Beginning in 1998, MHDS developed a Disaster Preparedness Program and plan for its agencies. In case of a major disaster, MHDS has a number of responsibilities dealing with officially declared disasters. Those responsibilities are identified in the Nevada Emergency Management Statewide Plan, which is coordinated and implemented by the Nevada Division of Emergency Management (DEM).
Workforce Recruitment and Retention - Especially in Rural Nevada
Retaining effective mental health professionals, especially in the rural areas, continues to be a major concern which directly affects MHDS capacity to provide services. According to a recent report (Behavioral Health Workforce-Fact Sheet, 2006), Nevada’s rural professional staff vacancy rate is 22%. 15 of Nevada’s 17 counties are designated as mental health shortages area(s). Between 2002 and 2012, Nevada’s general workforce will increase by 40.7%.
To address these concerns, MHDS is joining forces with the Western Interstate Collaborative for Higher Education to develop a model which can be used in Nevada to assist in the recruitment and retention of mental health professionals in rural and remote areas.
Data Sources and Suggested Readings
MHDS website: http://mhds.state.nv.us
Suicide Prevention Resource Directory (2003), MHDS, http://mhds.state.nv.us/admin/suicideprevent.shtml.
Mental Health Needs Assessment Report (2004), MHDS, http://mhds.state.nv.us/pdfs/NeedsAssessment2004.pdf.
Mental Health Prevalence Report (2004), MHDS, http://mhds.state.nv.us/pdfs/Prevalencestudy.pdf.
Budget Highlights Report (2005), MHDS, http://mhds.state.nv.us/pdfs/2005BudgetHighlights.pdf.
How Nevada Stuck Up (2005), MHDS, http://mhds.state.nv.us/pdfs/HowNevadaStacksUp2005.pdf.
Legislative Council Bureau Interim Study 05-8: Nevada Mental Health Plan Implementation Commission, http://www.leg.state.nv.us/lcb/research/05InterimReports/Bulletin05-08.pdf.
Mental Health Rural Clinics Organization Chart 2003, MHDS, http://mhds.state.nv.us/pdfs/ClinicOrgChart030205.pdf.
MHDS Decision Matrix Project for Atypical Anti-psychotics, MHDS, http://mhds.state.nv.us/pdfs/MHDSDecisionMatrixProject.pdf.
MHDS Formulary, MHDS, http://mhds.state.nv.us/pdfs/MHDSFormulary.pdf.
MHDS General Financial Overview for Fiscal Year 2003, MHDS, http://mhds.state.nv.us/pdfs/MHDSFormulary.pdf.
Monthly Report for Fiscal Year 2006, MHDS, http://mhds.state.nv.us/pdfs/Monthly2006.pdf.
Mortality Analysis Among Adult Mental Illness Clients in Nevada from 1998-2000, MHDS, http://health2k.state.nv.us/nihds/publications/Mental%20Health%20Report%202%20revised.pdf.
New Generation Psychiatric Medications in Nevada - 2003, MHDS, http://mhds.state.nv.us/pdfs/NGM2003.pdf.
Performance Indicators for Fiscal Year 2005, MHDS, http://mhds.state.nv.us/pdfs/PerformanceIndicators2005.pdf.
Pharmacy Management Allocation Plan Fiscal Year 2004, MHDS, http://mhds.state.nv.us/pdfs/PharmacyMAP2004.pdf.
Strategic Plan 2004 Through 2007, MHDS, http://mhds.state.nv.us/pdfs/StrategicPlan2004.pdf.
Study of Suicide Prevention from the 72nd Session of the Nevada Legislature, http://mhds.state.nv.us/pdfs/LCBSuicidePreventionStudy.pdf.
Study of the Feasibility of Adopting a Program of Outpatient Civil Commitment for Persons Who Are Mentally Ill, http://mhds.state.nv.us/pdfs/LCBSuicidePreventionStudy.pdf.
Web Site Statistical Report, MHDS, http://mhds.state.nv.us/pdfs/WebSiteStatisticalReport.pdf.
Behavioral Health Workforce-Fact Sheet (2006). (Nevada Western Interstate Collaborative for Higher Education, Denver CO).
Center for Mental Health Services (1999). Comprehensive community mental health services for children and their families program, annual report to Congress, 1999. Rockville, MD: Substance Abuse and Mental Health Services Administration.
Chanslor, P. (1968) History of the Nevada State Hospital (Reno: University of Nevada Press).
Coffey, R.M., M ark, T., King, E., Harwood, H., McKusick, D., Genvardi, J. et al (2000) National Estimates of Expenditures for Mental Health and Substance Abuse Treatment, 1997 (Report SMA-00-3499. Substance Abuse and Mental Health Services Administration).
Crowe, K. Center for Mental Health Services (2006). Comprehensive C ommunity Mental H ealth Block Grant Application (Rockville, MD: Substance Abuse and Mental Health Services Administration).
Crowe, K. (2006). Emergency Room Wait List, Nevada Division of Mental Health & Developmental Services, Carson City, NV.
“Children With Serious Emotional Disturbance; Estimation Methodology,”Federal Register (July 17, 1998, Vol. 63, No. 137).
“Grading the States: A Report on America’s Health Care System for Serious Mental Illness,” National Alliance on Mental Illness (March 2006).
“Estimation Methodology for Children With a Serious Emotional Disturbance” (SED), Federal Register (October 6, 1997, Vol. 62, No. 193).
Executive Order 13263: New Freedom Commission on Mental Health. Federal Register 67 (86, May 3, 2002).
Facts About The New StatePsychiatric Hospital in Las VegasValley, (2004). (Carson City NV: Nevada Division of Mental Health & Developmental Services).
Holzer, C. (2004). Synthetic Prevalence Estimates Model (Department of Psychiatry, University of Texas Medical Branch , 301 University Blvd., Galveston, Texas).
Kessler, R.C., Berglund, P.A., Zhao, S., Leaf, P.J., Kouzis, A.C., Bruce, M.L., Friedman, R.M., Grosser, R.C., Kennedy, C., Narrow, W.E., Kuehnel, T.G., Laska, E.M., Manderscheid, R.W., Rosenheck, R.A., Santoni, T.W., & Schneier, M., “The 12-Month Prevalence and Correlates of Serious Mental Illness (SMI),” (1996). Pp. 59-70 in Manderscheid RW and Sonnenstein MA (Eds.) Mental Health (Washington, DC: United States Government Printing Office).
July 1 2003 Estimates (2003), Nevada State Demographer.
Brian Lahren (1995). Nevada’s Mental Health System, 1960 to 1994, With Recommendations for Improvement. Nevada Public Affairs Review. Lahren B. (1995). Nevada’s Mental Health System, 1960 to 1994, With Recommendations for Improvement. Nevada Public Affairs Review.
Mental Health: United States Public Health Service. Office of the Surgeon General, National Institute of Mental Health United States. Substance Abuse and Mental Health Services A dministration. Center for Mental Health Services.
Pillard, E. (1979). “Nevada’s Treatment of the Mentally Ill,” Nevada Historical Society Quarterly, Vol. XXII.
Overview of Plans for the New Psychiatric Hospital in Las Vegas (2004). (Carson City NV: Nevada Division of Mental Health & Developmental Services).
Public Law 102-321. (July 10, 1992). p. 106 STAT 347.
Rice, D.P., & Miller, L.S. (1996). “The Economic Burden of Schizophrenia: Cnoceptual and Methodological Issues and Cost Estimates.” Pp. 321-334 in M . Moscarelli, A. Rupon and N. Sartorious (Eds.) Schizophrenia (Chickchester UK: Wiley).
State Profile Highlights (2005). National Association of State Mental Health Program Directors Research Institute, Inc. (NRI) No. 05-08. November 2005.
U.S. Department of Health and Human Services. (1999). Mental Health: A Report of the Surgeon General. Rockville, MD.
Valentine, L. (2004). 2004 Needs Assessment (Carson City: Nevada Division of Mental Health and Developmental Services).
Valentine, L., and Karr D. (2005). How Nevada Stacks Up 2005 (Carson City: Nevada Division of Mental Health and Developmental Services, MHDS).
Valentine, L., and Karr D. (2005). Prevalence Study, MHDS.
Williams, Troy. (2004). MHDS Caseload & Projections (Carson City NV: Nevada Division of Mental Health and Developmental Services).
Witkin, M. J., et al. (1998). In R. W. Manderscheid and M. J. Henderson (Eds.), Mental health, United States 1998 (pp. 143-169). Rockville, MD: U.S. Department of Health and Human Services.
World Health Organization. (1996). The Global Burden of Disease. Washington, DC.
Community Resources
Adult Services:
Mental Health & Developmental Services (MHDS), 505 East King Street, Room 602, Carson City, Nevada 89701-3790. Tel. 775-684-5943, Faxes 775-687-5966 & 775-687-5964.
Lakes Crossing Center For The Mentally Disordered Offender, 500 Galletti Way, Sparks, Nevada 89431-5573; Tel. 775-688-1900, Fax 775-688-1909.
Northern NV Mental Health Services (NNAMHS), 480 Galletti Way, Sparks, Nevada 89431-5573. Tel. 775-688-2001, Fax 775-688-2092.
Southern Nevada Adult Mental Health Services (SNAMHS), 6161 West Charleston Boulevard, Las Vegas, Nevada 89146-1126. Tel. 702-486-6000, Fax 702-486-6248.
SNAMHS - Henderson Office, 98 East Lake Mead Drive, Henderson, Nevada 89015. Tel. 702-486-6700, Fax 702-486-708.
SNAMHS - North Las Vegas Office, 2121 North Las Vegas Boulevard, North Las Vegas, Nevada 89030. Tel. 702-486-5750. Fax 702-486-5769.
SNAMHS - Southeast Office, 1820 East Sahara Avenue, Ste 109, Las Vegas, Nevada 89104-3736. Tel. 702-486-8289. Fax 702-486-8295.
Rural Clinics Community Mental Health Centers- Admin Ofc., 503 N. Division St., Carson City, NV 89703. Tel. 775-687-1000.
Rural Clinics:
Battle Mountain Mental Health Center, 101 Carson Road, Suite #1/P.O. Box 50, Battle Mountain, NV 89820-0050. Tel. 775-635-5753, Fax 775-635-8028.
Hawthorne Mental Health Center , 1000 “C” Street/P. O. Box 12, Hawthorne, NV 89415-0012. Tel. 775-945-3387, Fax 775-945-2307.
Carson Mental Health Center, 1330 South Curry Street, Carson City, NV 89703-5202. Tel. 775-687-4195 and 775-687-5103.
Lovelock Mental Health Center, 775 Cornell Ave. Suite #C, Lovelock, NV 89419-1046. Tel. 775-273-1036, Fax 775-0273-1109.
Dayton Mental Health Center, 120 Pike Street/P.O. Box 1597, Dayton, NV 89403-1597. Tel. 775-246-5240, Fax 775-246-5364.
Mesquite Mental Health Center, 61 N Willow Suite 4 /P.O. Box 3567, Mesquite, NV 89024 . Tel. 702-346-4696, Fax 702-346-4699.
Douglas Mental Health Center, 1538 HWY 395 N, Gardnerville, NV 89401-5239 (P.O.Box 1509, Minden, NV 89423-1509). Tel. 775-782-3671, Fax 775-782-6639.
Pahrump Mental Health Center, 1840 S. Pahrump Valley Blvd., Pahrump, NV 89048. Tel. 775-751-7406, Fax 775-751-7409.
Elko Mental Health Center, 1515 7th Street, Elko, NV 89801-2558. Tel. 775-738-8021, Fax 775-738-8842.
Silver Springs Mental Health Center, 3595 Highway 50 East, Springs, NV 89429-1136. Tel. 775-577-0319, 775-577-9571.
Ely Mental Health Center, 1665 Avenue F/P.O. Box 151107, Ely, NV 89315. Tel. 775-289-1671, Fax 775-289-1699.
Tonopah Mental Health Center , 825 S Main P.O. Box 494, Tonopah, NV 89049-0494. Tel. 775-482-6742, Fax 775-482-3718.
Fallon Mental Health Center, 151 North Main Street, Fallon, NV 89406-2909. Tel. 775-423-7141, Fax 775-423-4020.
Winnemucca Mental Health Center , 3140 Traders Way/P.O. Box 230, Winnemucca, NV 89446-0230. Tel. 775-623-6580, Fax 775-623-6584.
Fernley Mental Health Center, 115 West Main Street/P.O. Box 2314, Fernley, NV 89408-231 4. Tel. 775-575-0670, Fax 775-575-0672.
Yerington Mental Health Center , 310 Surprise Avenue, Yerington, NV 89447-2542. Tel. 775-463-3191, Fax 775-463-4641.
Laughlin Mental Health Center, 3650 So. Pointe Circle, Suite 208, Laughlin, NV 89028. Tel. 702-298-5313.
Mojave Mental Health Services. Nonprofit outpatient services (formed in collaboration with the University of Nevada School of Medicine), www.mojave.org. 6375 W. Charleston Blvd., Las Vegas, NV 89146. Tel. 702-968-4000.
Montevista Hospital. Private psychiatric facility with residential and outpatient services. 5900 W. Rochelle Ave., Las Vegas, NV 89103. Tel. 702-364-1111.
NAMI of Nevada . Education and support group for consumers of mental health services and their families. 1170 Curti Dr, Reno, NV 89502; Tel. 775-329-3260; Southern Nevada, Tel. 702-363-9584.
The Salvation Army . Nonprofit offering behavioral and rehabilitation services. 35 W. Owens, Las Vegas, NV; Tel. 702-649-8240; 1932 Sutro St., Reno, NV 89512. Tel. 775-688-4555.
Veterans Affairs Administration. Facilities . Hospital/Ambulatory Clinic. Statewide: Tel. (800 ) -827-1000; 1000 Locust St, Reno, NV 89502. Tel. 775 -786-7200; 4700 N. Las Vegas Blvd, Nellis AFB, Las Vegas, NV 89146. Tel. 702-653-2222; 6 Steptoe Circle, Ely, NV 89301. Tel. 775-289-3612.
WestCare. Nonprofit behavioral healthcare with residential and outpatient services, http://www.westcare.com; 5659 Duncan Drive, Las Vegas, NV 89108. Tel. 702-385-2020. WestCare Community Triage Center, Las Vegas. Tel. 702 -383-4044.
West Hills Hospital. Private psychiatric facility with residential and outpatient services. 940 E. Ninth St ., Reno, NV 89512. Tel. 775-323-0478.
Children Services:
Nevada Division of Child & Family Services . State children’s mental health agency, http://dcfs.state.nv.us, 711 E. 5th St, Carson City, NV 89701. Tel. 775 -684-4400; Southern Nevada Child and Adolescent Services, 6171 W. Charleston Blvd, Bldg 8, Las Vegas, N V 89146. Tel. 702 -486-6120.
Northern Nevada Child and Adolescent Services, 2655 Enterprise Rd, Reno, NV 89512. Tel. 775-688-1600.
Desert Willow Treatment Center, 6171 W. Charleston Blvd, Bldg 17, Las Vegas, NV 89146. Tel. 702-486-8900.
Montevista Hospital. Private psychiatric facility with residential and outpatient services. 5900 W. Rochelle Ave., Las Vegas, NV 89103. Tel. 702 -364-1111.
Nevada PEP. Nonprofit educational and support center for children with disabilities, http://www.nvpep.org; statewide tel. 800-216-5188; 2355 Redrock St, Suite 106, Las Vegas, NV 89146. Tel. 702 -388-8899; 4600 Kietzke Lane, Suite O-269, Reno, NV 89502. Tel. 775-448-9950.
Spring Mountain Treatment Center. Behavioral health treatment for children and adolescents, www.springmountaintreatmentcenter.com, 7000 Spring Mountain Rd, Las Vegas, NV 89117. Tel. 702-873-2400, www.springmountaintreatmentcenter.com.
WestCare. Nonprofit behavioral healthcare with residential and outpatient services, 5659 Duncan Drive, Las Vegas, NV 89108. Tel. 702-385-2020, http://www.westcare.com.
This report was prepared by Kathryn Landreth, former Legal Advisor to the Las Vegas Metropolitan Police Department and former United States Attorney for the District of Nevada in collaboration with Carlos Brandenburg, Ph.D., Division Administrator, Nevada Division of Mental Health & Developmental Services, and Dr. Simon Gottschalk, Associate Professor, Department of Sociology, University of Nevada Las Vegas.
To contact Kathryn Landreth, please write to P.O. Box 8253 Reno, NV 89507, Email: klandreth@tnc.org. To reach Simon Gottschalk, write to Department of Sociology, University of Nevada Las Vegas, 4505 Maryland Parkway, Box 455033, Las Vegas, NV 89154-5033. Telephone: 702-895- 0266. Email: karma@unlv.nevada.edu. To contact Dr. Brandenburg, write to NV Division of Mental Health & Developmental Services, 505 E King St., Suite 601, Carson City NV. Telephone: 775-684-5943 Email:
cbrandenburg@mhds.nv.gov.
Special thanks are due Kevin Crowe, Ed.D, Chief of Planning and Evaluation, Nevada Division of Mental Health and Developmental Services, for his valuable suggestions and additions to this report.